In this article, I will aim to answer all your questions as to whether or not YOU need an MRI scan for sciatica.
Aims of this post:
- To clarify when an MRI scan for sciatica is the right way forward, and when it isn’t
- To discuss the pro’s and con’s of MRI scans
- To talk about what to expect on the results of your MRI scan – what’s “normal”?!
Before we dive in, please be aware that we are part of the Amazon Affiliate programme. This page may contain Amazon affiliate links, so if you choose to purchase a product for your sciatica that we recommend through a link on this page, we will receive a small commission at no extra cost to you. This helps us keep Overcome Sciatica alive! Thank you for your support. Please be assured that we only ever recommend products that we truly believe can help.
One of the most common questions that I get asked when I am treating people who are trying to get rid of sciatica is this:
How can you be sure of what’s causing my sciatica without a scan?
The answer is simple: I can’t.
Not even the most experienced, well qualified, sciatica-specialist doctor can be 100% sure what is causing your sciatica without some form of diagnostic procedure.
However, not everyone needs an MRI scan for sciatica, and it would actually be detrimental to a large pocket of people within this population to have a scan. I’ll explain exactly why very shortly.
First of all, if you need a refresher of what sciatica is, what causes it and why you are experiencing the symptoms that you currently feel, read this article HERE.
When we talk about an MRI scan for sciatica, we are referring to Magnetic Resonance Imaging (MRI scan for short).
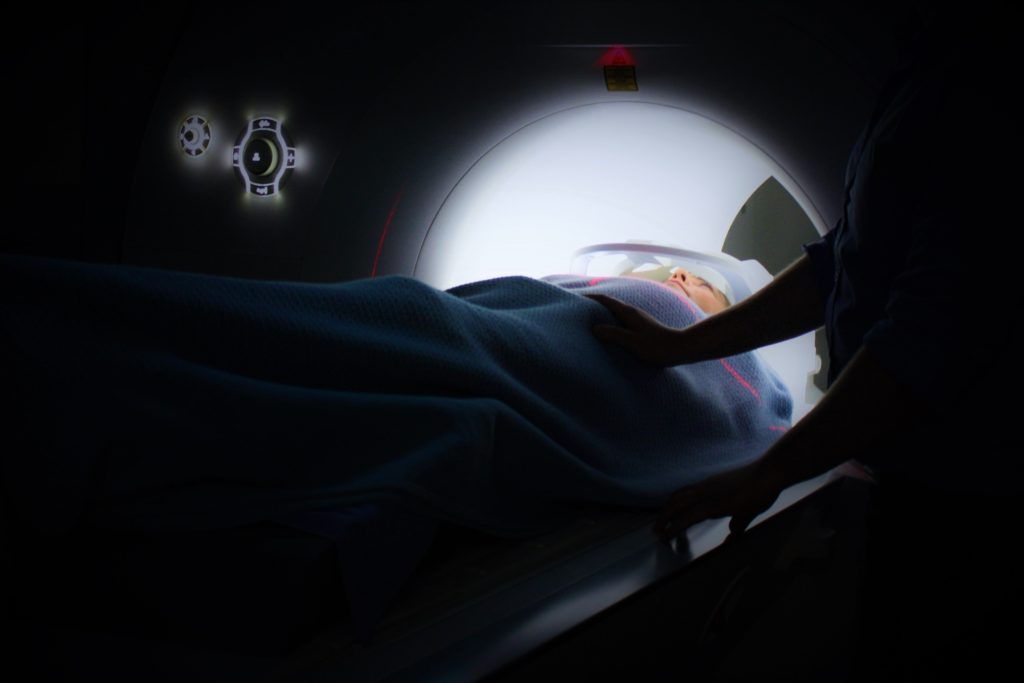
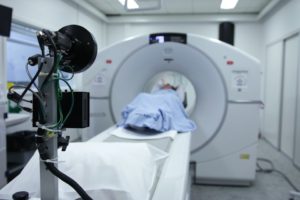
These are the scans that take place in the big machines, where you lay on a bed and travel into a big contraption that looks like something from Star Trek.
They take around 40 minutes to complete and at the end, the radiologist will have a large collection of “snap shot” images from your spine.
The way they work is by measuring magnetic fields. The scanner will send a magentic “signal” through your body as you go through the scanner, which will be picked up on the other side of the machine.
Different tissues in the body will reflect the differences in the magentic signal that is picked up. The differences in the tissues can be seen on the images at the conclusion of the scan.
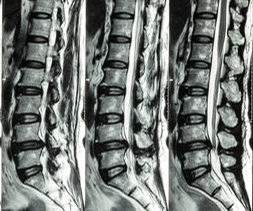
When you have an MRI scan for sciatica, usually the lower back and pelvis is the “target” area for the scan.
These scans are a phenomenal invention as they allow us to see structures like nothing we had before.
On an X-ray, you can only make out bone, not soft tissue. Whereas with an MRI scan for sciatica, you can see bone, muscle, soft tissue, nerve and spinal cord, all through a series of images which are like little cross sections through your body.
These scans are incredibly useful in a multitude of ways throughout the medical profession.
The problem is that these MRI scans are so good that they pick up absolutely everything in the scanned region. It is like one area of your body being examined under a fine microscope.
“So isn’t that a good thing?” I hear you ask.
Well, yes… and no.
The reason for the “no” is that no one’s spine is perfect. Especially seeing as after we reach the age of 20, our bodies are technically in decline due to the aging process (depressing, I know!)
Someone once used an analogy that stuck with me with regards to MRI’s:
An MRI scan for sciatica is like taking your car into a formula one garage; even though your car still functions well, the mechanics are going to find lots of little problems with it.
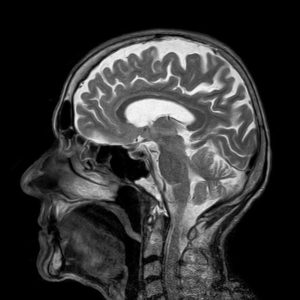
Therefore, on an MRI scan for sciatica, we are likely to see every little “fault” in our spines. We might see degenerating discs, worn facet joints, little cysts, one vertebrae slipping on top of another one and other changes due to general use of our bodies throughout the course of our lives.
The thing is, all of these changes are normal. Mostly everyone will have some of these changes going on in their spine, whether they are with or without pain.
Here is a great video that explains this further. Everyone should watch this video:
A few facts for you; a study was done in 2014 by Brinjikji and colleagues, who pooled data from loads of studies that scanned people’s spines when they had no pain. These people were between the ages of 20-80 years old. The researchers documented all of the “abnormal” findings on the MRI scans from each of these studies. Remember, all the participants were asymptomatic.
The researchers found that, out of 3,110 people:
-
Up to 96% of them had disc degeneration.
-
There were disc bulges in 30% of the 20 year olds, and 84% of the 80 year olds.
-
The disc was actually protruding from the spine in up to 43% of people.
-
There was some evidence of “wear and tear” in nearly everyone!
So, as we can see from the fact that all these findings are seen in pain-free people, an MRI scan for sciatica can be very good at telling us what is worn or not pristine in our spines, but it has no way of showing the CAUSE of someone’s pain, and will give us no indication of what to do to get rid of the sciatica that someone is suffering with.
There is no big red arrow pointing to the cause of the problem! How easy life would be if that were true.
Are You Looking for RAPID Relief from Sciatica?
My good friend, colleague and fellow international sciatica expert, Dean Volk, has a brand new sciatica relief video course available – and I’m delighted to be an official sponsor!
Check out Dean Volk’s “Kicking Sciatica OUT of the Butt!” Online Pain Relief Course Here!
I can proudly recommend Dean and his course for sciatica sufferers – because I’ve seen his incredible results first-hand. You can check out his course (and get lifetime access to the videos and bonus content) by clicking HERE.
So even after an MRI scan for sciatica, it is the GUESSWORK of the clinician as to what problem within that scan is the cause of someone’s sciatica.
We know that sciatica is caused by something irritating the sciatic nerve, usually either in the lower back or the hip. Usually, we can make a very accurate educated guess as to what is causing the sciatic pain that you feel based on the symptoms that you are experiencing.
Clues like the things in your life that aggravate the pain, the things you can do to ease the pain, how the pain first started and how severe it is all paint us a picture of the likely cause of your sciatica.
As previously mentioned in the article What Is Sciatica – The Ultimate Guide, I described how very rarely something more sinister (like a tumour or an illness like TB) can be the cause of a person’s sciatica.
Now to be clear, we are talking about a fraction of people less than 1% of the total population that suffer from sciatica, so a very small number.
Even still, there was a time when lots and lots of people who had sciatica were getting sent through by their doctors for an MRI scan for sciatica, just to rule out the more urgent causes. This worked pretty well in terms of identifying the unlikely cancers and other nasties, but there was a big problem.
Rates of surgery shot up.
People were sent to consultants very quickly after feeling the first twinges of sciatica.
If a moderate disc bulge was seen, a surgical opinion was requested.
Now this might not sound like a bad thing, until you hear the following stat:
Spinal surgery for sciatica is only successful in roughly ONE THIRD of cases.
A third of people get no better, and the other third actually get worse.
So overall, the outcome of sending everyone for an MRI scan for sciatica as soon as they developed pain was a glut of unnecessary surgeries (in people that had a good chance of getting rid of sciatica without surgery), huge cost on the healthcare system, massive rates of morbidity and people left disabled by rods, nails and screws in their back.
Not to mention the fact that lots of people had surgery on things that probably weren’t even causing them pain in the first place!
Not good!
Now, please don’t get me wrong, MRI scans for scans are still incredibly useful in SOME instances. They can help to rule out serious problems, when there is cause to believe that there is something sinister going on, and they can also help to identify why something hasn’t recovered as expected after all reasonable methods have failed.
Below is a guide to when I personally would recommend that one of my clients gets a scan. Obviously, this is just my opinion of when a scan is necessary; other clinicians’ opinions may vary.
To read more about surgery for sciatica, click here!
The Situations When You Likely Need An MRI Scan for Sciatica
If you have problems with your bladder or bowel
This can indicate a compression of the cauda equina – a bundle of nerves that makes up the lowest part of the spinal cord. If you are either struggling to initiate the flow of urine, or have had an accident, you certainly need attention straight away. For this one, call your doctor immediately or make the trip to accident and emergency as this problem needs sorting quickly.
If you have numbness in your “saddle” area
Again, this can indicate a cauda equina compression. Don’t delay for this one, either.

If you feel that your muscles in your legs are getting weaker, or your knees, hips or ankles want to give way when you walk
This is certainly something I would want investigated. This type of complaint can suggest that one of the nerve roots is almost completely compromised in the spine, and as a result the muscle it supplies can’t do its job correctly. This will present as weakness in one or more muscle groups in your legs.
If you have a past history of cancer and you develop sciatica
Unfortunately, a past history of cancer is a high risk factor for developing cancer again. Sometimes, especially after bowel or bladder cancer, there can be a recurrence that manifests as a tumour in the spine which compresses a nerve root, causing sciatica.
If you have not had cancer before, your sciatica is very unlikely to be caused by cancer! If you have, make sure you get checked out; chances are you’ll be OK, but the quicker you know, the quicker it can be sorted.
I have a relatively low threshold for suspicion with people who have had cancer before and would be more likely to send them through for an MRI scan for sciatica.
If you have sudden weight loss, night sweats or begin feeling generally unwell alongside sciatica
This can indicate the start of one of a few serious illnesses, which can manifest as painful sciatica. Again, unlikely; but best to get checked out if you have any of these symptoms.
If you have osteoporosis, felt a “drop” in your spine, or have sciatica as a result of trauma to that area
Traumatic sciatica can be caused by something more serious like a fracture, which may need an intervention.
Even without significant trauma, a fracture can occur in osteoporosis so it’s best to get checked out just to be sure.
Most people who have osteoporosis are over the age of 65. You can be diagnosed with osteoporosis if you have regular fractures after minimal trauma, or if you undergo a DEXA bone density scan.
You can counter the effects of osteoporosis by making sure you are consuming plenty of calcium, such as milk and other dairy products.
If you’ve tried everything, like treatment from a healthcare professional, rest, exercise, correct positioning techniques and good lifestyle changes and your sciatica is STILL no better after 12 weeks
In this instance, it is definitely worth an investigation just to work out why the recovery process has been so delayed. Most people (90%) get better within 12 weeks, so hang on in there. It may be that your body is just taking its time in sorting this problem out, or that your original problem has healed but you have remained really stiff and that’s preventing a recovery.
Hint: Check this article HERE for methods of making your work place more sciatica-friendly, helping you to recover quicker from a flare-up.
If someone is really frightened, anxious or scared about their sciatica
I have certainly recommended to lots of people suffering from significant anxiety that they get an MRI scan for sciatica – but this isn’t the right way forward for everyone. Sometimes, scanning the back in situations like these can make a person’s anxiety worse. However, being told that you have not got cancer, nor a fracture or strange exotic disease, and that it is likely to get better with a bit of time and some treatment, can do someone the world of good.
Summary
As is true with any decision that needs to be made involving a person, there are exceptions to every rule and lots of grey areas. I think the key takeaway from this post is that it is important to bear in mind that an MRI scan for sciatica can actually do more harm than good in some instances, however a scan may be the correct route forward for some people.
If you’ve enjoyed this post, please be sure to pass it onto someone else who may benefit from the information I’ve shared today.
As always, thanks for reading.
The information on Overcome Sciatica should never be used as a substitute for medical advice from a doctor. Never put into action any tips or techniques from Overcome Sciatica without checking with your doctor first. Please see full terms of use here.






thank you for sharing this informations
Thank you so much. I had my MRI results and it came back negative. Shoot pains from the lower back, testicular, and both of my feet. I am very discouraged. I’m 36 years old and have been dealing with these pains since 2014