Without being an expert, it’s often extremely difficult to tell exactly whether it is sciatica or piriformis syndrome causing that pain in your leg.
And I don’t just mean that it’s difficult for YOU to tell – I also mean difficult for doctors or physiotherapists too! There’s often not a clear picture when we try to work out what’s causing someone’s leg pain, and the symptoms from different causes can look incredibly similar.
I would ultimately recommend that anyone asking this question about their own leg pain gets assessed by a professional first – we have some techniques that we can use to help diagnose these issues in a face-to-face appointment.
However, today I want to give you a brief outline of the difference between sciatica and piriformis syndrome, as it pays to know what’s causing your problem before you attempt to treat it at home.
Before we dive in, please be aware that we are part of the Amazon Affiliate programme. This page may contain Amazon affiliate links, so if you choose to purchase a product for your sciatica that we recommend through a link on this page, we will receive a small commission at no extra cost to you. This helps us keep Overcome Sciatica alive! Thank you for your support. Please be assured that we only ever recommend products that we truly believe can help.
So, Do I Have Sciatica or Piriformis Syndrome?
I often get asked: “I’ve got this horrible leg pain that hurts like hell. How can I tell if it’s sciatica or piriformis syndrome?”
There’s a lot to unpick in this question, but I’ll do my best to explain it to you here.
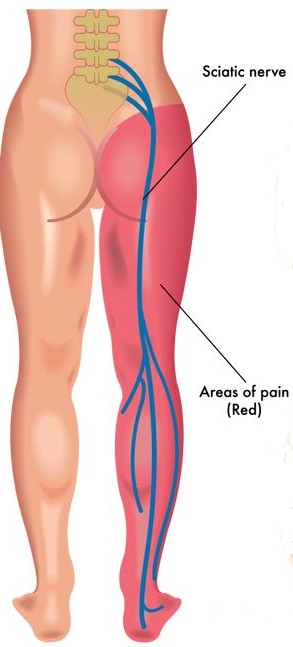
First, let’s talk about sciatica. Sciatica isn’t actually a disease or pathology. Sciatica simply describes the SYMPTOM of nerve pain in the leg.
This means that many problems will give you ‘sciatica’ (remember, this just means nerve pain in the leg), including disc problems, arthritis of the spine and, yes, piriformis syndrome.
So really, it’s possible that you could have sciatica CAUSED BY piriformis syndrome. Or it could be caused by something else entirely.
What most people mean when they ask whether it’s sciatica or piriformis syndrome causing their problem is whether it’s a problem in their back or the piriformis muscle that’s causing the issue.
How is Sciatica Caused by the Lower Back?
To simplify things, there are 2 main classifications of lower back problems that can cause sciatica.
#1: Disc bulges, herniations and prolapses
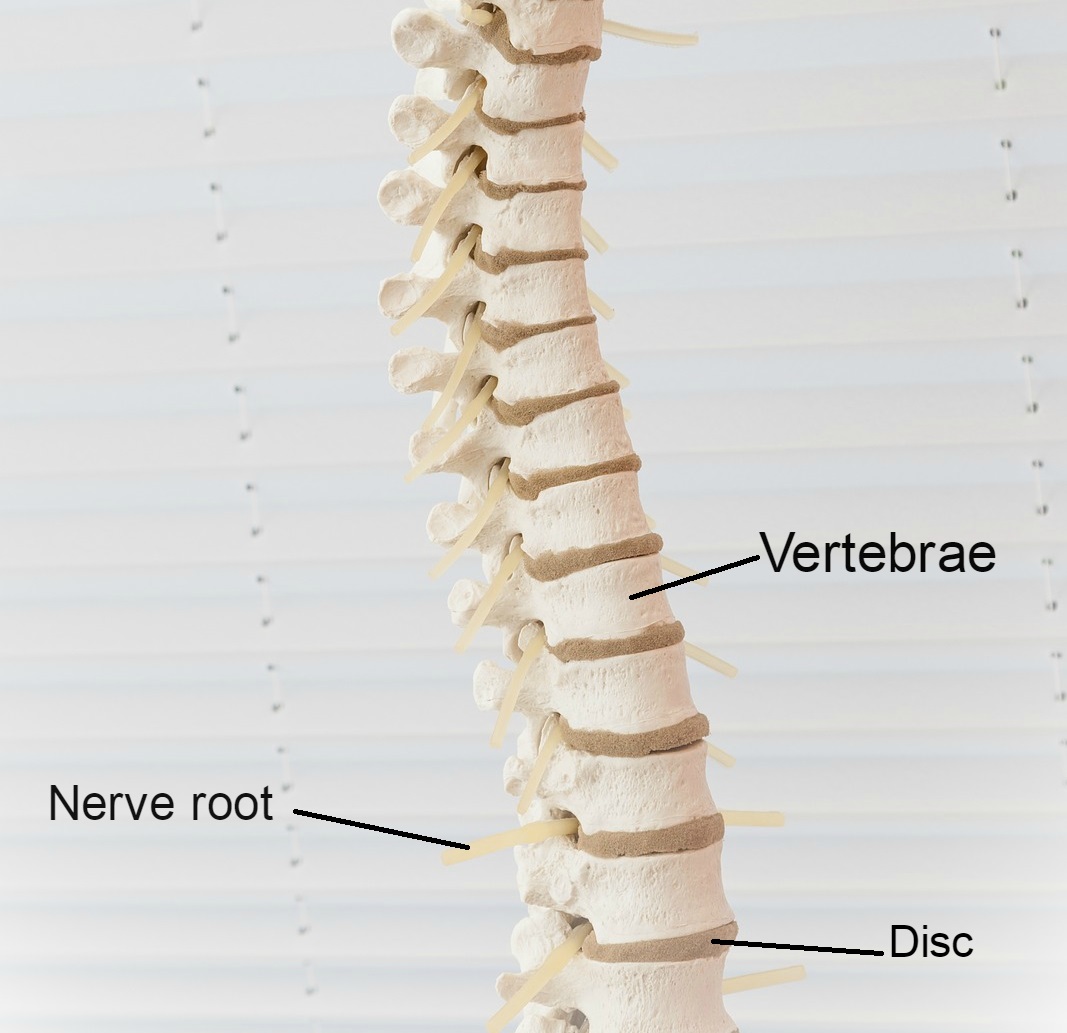
We have 5 lumbar vertebrae (bones in the lower back) plus 1 sacrum (tail bone).
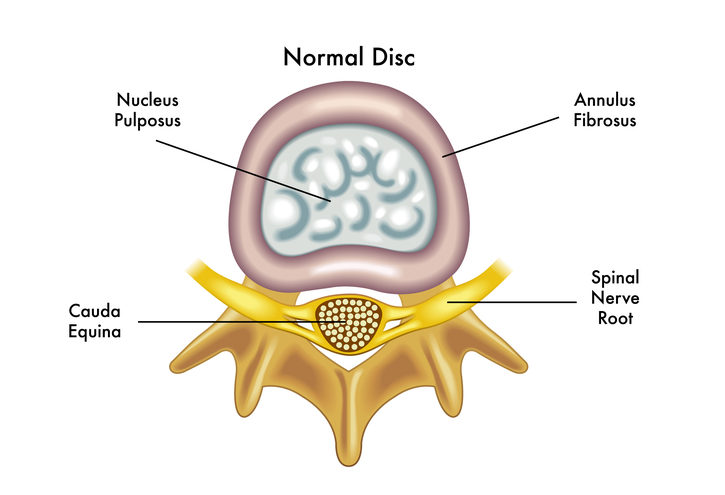
Between each one of these vertebrae are the intervertebral discs. Each disc is made up of a soft inner section – called the nucleus – and a tough outer section made of cartilage called the annulus.
The tough outer part of the discs can develop tiny tears over time through repetitive movements under load. These micro-tears can sometimes develop into “bulges”, which occur when pressure causes the inner material in the disc to push into these weakened zones. It’s important to note that in 90% of cases, disc bulges don’t cause any problems whatsoever.
I likely have a load of disc bulges from various sports and the gym work that I do, yet I don’t suffer from back pain or sciatica.
However, sometimes these bulges can encroach on the tight spaces that the nerves run through. In a worst case scenario, the inner material of the disc can actually leave the side of the disc through these weakened areas, causing a painful chemical reaction around the nerve root. This leads to the symptoms of sciatica and is called a disc herniation or prolapse (same thing, different name).
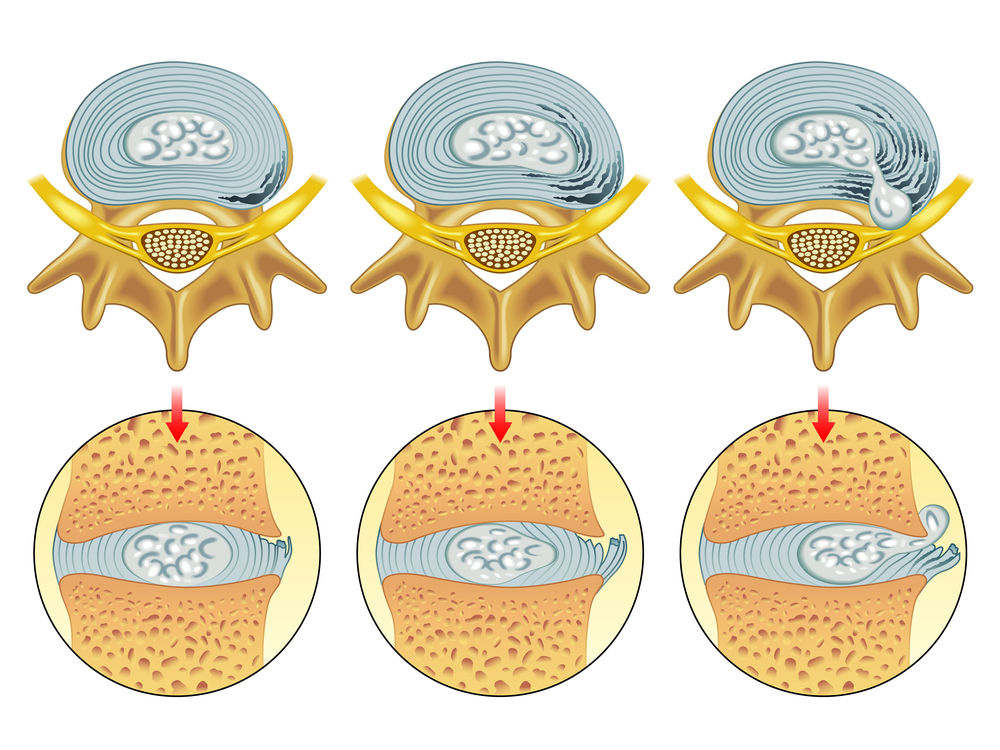
This often gets worse when a person bends forward, as pressure on the front of the disc causes the inner material to “bulge” backwards towards the nerve root, irritating it and causing sciatica symptoms.
#2: Age-related changes including arthritis, spinal stenosis and degenerative discs
As we age, our discs dry out and lose height, the bone around our joints thickens, our joints become stiffer and we lose the cartilage that helps to lubricate movement in our spines.
Sounds awful, right?
Actually, it rarely is!
Almost everyone has some degree of these changes in the spine once they are over the age of 30. In fact, studies have shown some signs of deterioration in OVER NINETY PERCENT of people aged 30+!
However, these studies were performed on people who DIDN’T have back pain or sciatica, so we know that aging changes are NOT directly correlated with pain.
However, in some people, these changes can cause a smaller and less lubricated space for the nerve roots to exit the spine from, which leaves them vulnerable to becoming compressed. This compression can cause sciatica.
In more severe cases, it leads to a condition called “spinal stenosis”.
This is characterised by very tight spaces where the nerves run through, causing them to be compressed whenever someone is walking or standing upright for any length of time. With this problem, the pain tends to go away as soon as they bend forward.
Are You Looking for RAPID Relief from Sciatica?
My good friend, colleague and fellow international sciatica expert, Dean Volk, has a brand new sciatica relief video course available – and I’m delighted to be an official sponsor!
Check out Dean Volk’s “Kicking Sciatica OUT of the Butt!” Online Pain Relief Course Here!
I can proudly recommend Dean and his course for sciatica sufferers – because I’ve seen his incredible results first-hand. You can check out his course (and get lifetime access to the videos and bonus content) by clicking HERE.
Now there are other problems that can cause sciatica, but most of them will fall into one of these two broad categories.
A slightly different cause of sciatica is piriformis syndrome. Let’s talk a bit about this now:
Piriformis Syndrome Causing Sciatica
Unlike the other causes of sciatica, piriformis syndrome actually has nothing to do with the lower back. Piriformis syndrome is primarily a problem to do with the hips.
We all have a muscle that sits deep in the buttock, called the piriformis. Its main job is to stabilise the pelvis as we walk, as well as helping to rotate the leg outwards when we need to do something like crossing our legs. It’s a very important muscle, and we’d struggle to walk, run or stand well without it.
In most people, the sciatic nerve travels past the piriformis, staying well clear of it on its path.
In some people (roughly 10% of the population according to recent studies), the sciatic nerve runs through the piriformis rather than past it. In these people, when the piriformis gets tight the sciatic nerve can become compressed, causing sciatica.
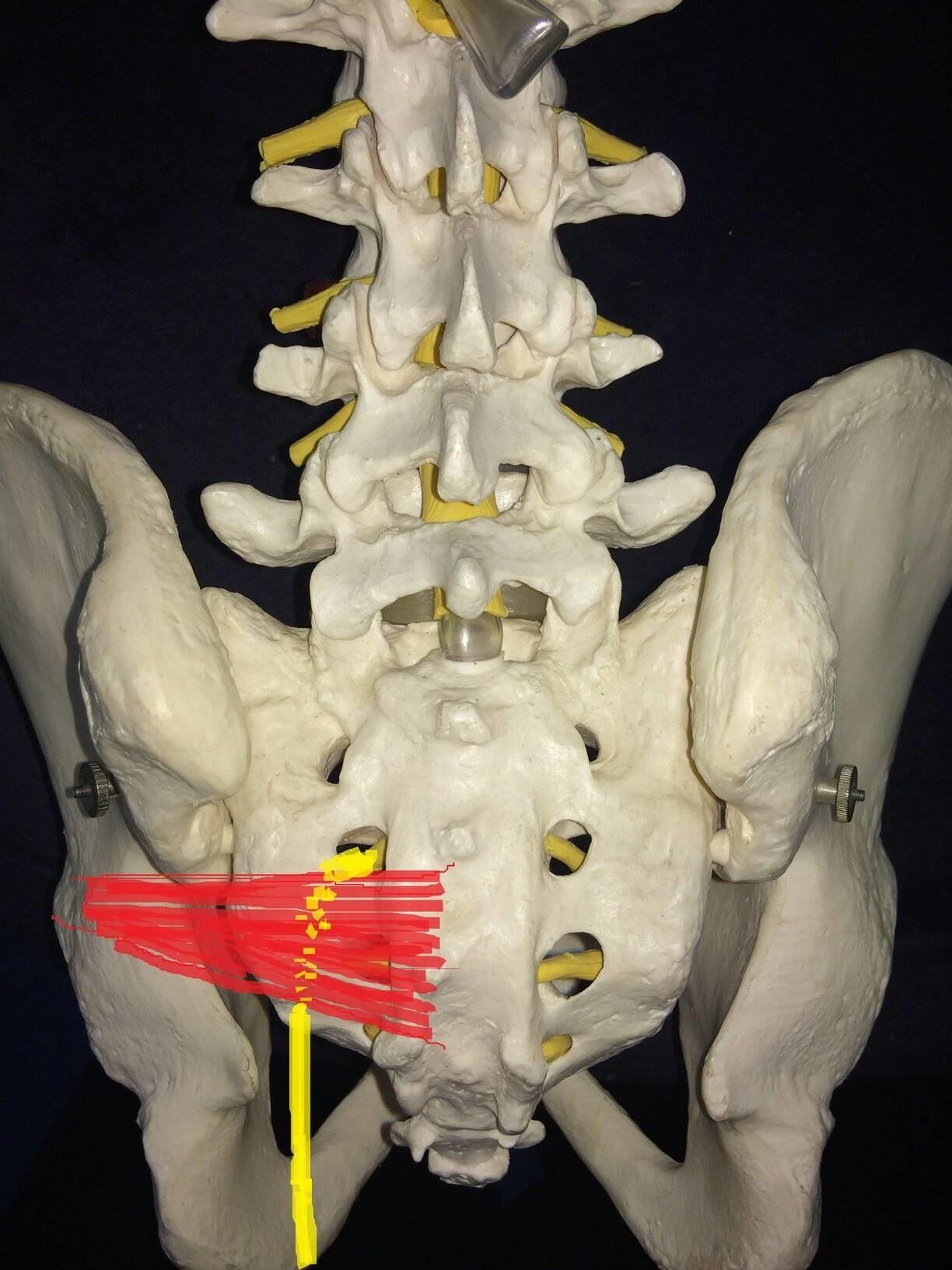
Now, the symptoms of sciatica caused by piriformis syndrome and a problem in the lower back are very similar on a lot of levels.
Both causes can give you pain all the way down to your foot, pins and needles, numbness and problems with certain positions.
However, there are some key differences.
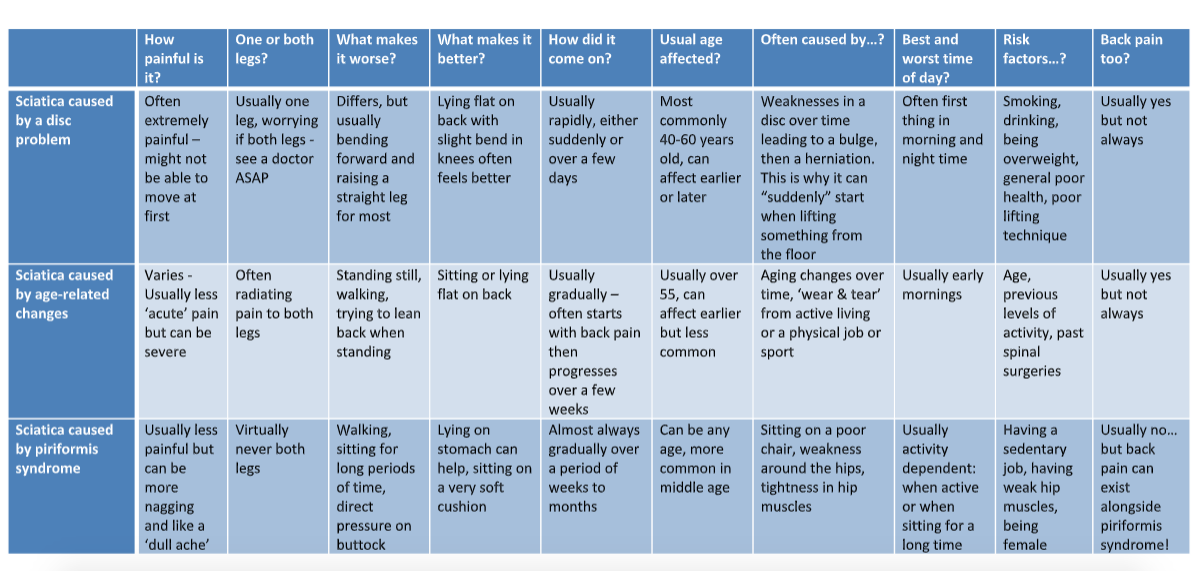
I’m going to lay these out for you in a handy reference table, then explain them one by one. Please remember I’m making generalisations here; there are no absolutes that apply to all – so please don’t use this guide as a substitute for seeing your doctor.
How painful are the conditions?
Usually, sciatica caused by a disc bulge, herniation or prolapse gives people the most ‘acute’ pain. A lot of my clients with this issue say that when it first happened, they were unable to move for a few days.
It can cause the classic “locked back” type symptom where you get “stuck” in one position for hours on end. Not pleasant.
Sciatica caused by ageing changes and piriformis syndrome can still be very painful, but because the conditions came on gradually, they are often more manageable.
The pain can be most ‘constant’, however, so these problems can be equally as troublesome.
One or both legs?
Sciatica usually affects just one leg and you should get a medical assessment as soon as possible in all cases if the pain affects both sides.
It is unfortunately common for ageing changes to lead to sciatica in both legs – which can make it difficult to treat.
If you suddenly developed sciatica in both legs, it could be that you’re suffering from a “central” disc bulge, which means the lowest part of the spinal cord is being compressed. This needs rapid assessment, so get checked out fast.
I’ve never come across a true piriformis syndrome in both legs – usually, one hip takes the brunt of the problem while the other one is spared.
What makes it worse?
Now, the answer to this question will be different for anyone that you speak to. However, there are some common trends.
The classic pattern we see with disc bulges is a problem with bending forward at the spine. This may bring on dramatic back pain and sometimes sciatica, too.
For almost all people with a disc problem behind their sciatica, trying to raise the affected leg straight up in the air when lying on your back will be very painful.
For people with ageing changes behind their sciatica, pain when walking and standing still is often the complaint, while sitting down tends to take the pain away.
Sitting can be a big problem in piriformis syndrome, but not for everyone. Often, active people like runners or cyclists develop piriformis syndrome and it can come on slowly as they run and cycle.
What makes it better?
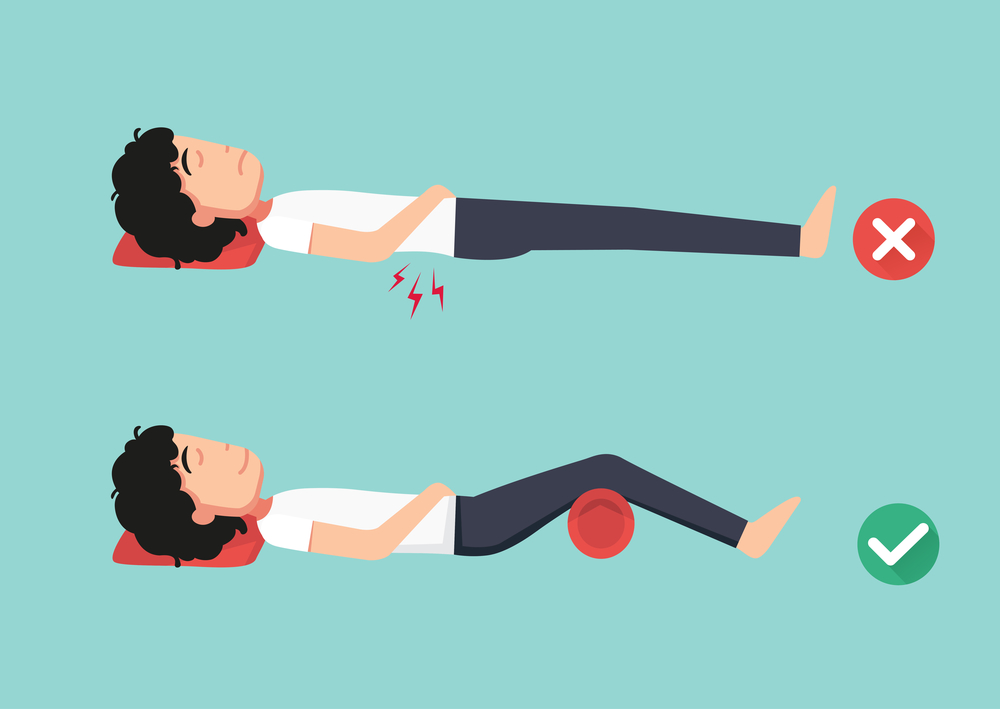
For a disc problem, most people find the following position quite comfortable:
This position takes a stretch off the nerve and helps the lower back to relax a bit.
For people with ageing changes, usually sitting or even just bending forward a bit is enough to alleviate their symptoms.
For piriformis syndrome, lying on your front is often enough to take the pain away.
How did it come on?
With a disc problem, the onset is usually rapid. It’s the classic case of trying to lift something heavy and your back and leg just ‘going’. The pain can start there and then, but the onset of pain can often be delayed by a few days.
With aging changes, the classic story is that the person started off with some back pain for a few months or even years but they’d managed to put up with it. Then, over a period of a few weeks to months, the pain gradually started in their leg too.
With piriformis syndrome, a slow onset of buttock pain might be the first complaint. This is often followed by leg pain which usually starts gradually, too.
Usual age affected?
For disc problems, the most common sufferer is a male in their 40’s through to their 60’s. I don’t know why men are affected more than women, but the ratio is about 60:40 from the latest figures.
For aging changes, the typical age is over 60, but I have known younger people to suffer from stenosis and other issues too. A lot of the likelihood of whether you’ll suffer this problem or not comes down to the occupation you’ve done throughout your life. The more laborious, the higher your chances.
However, it’s no reason to give up the trade early – active tradespeople benefit from higher general fitness and are less likely to suffer from heart disease and other cardiovascular killers.
Piriformis syndrome can affect either sex at any age, although there’s a trend towards women being affected more than men (probably due to the width of their hip bone structure compared to men’s – meaning the pelvis muscles have to work harder in women).
Often caused by…?
Although it might seem like disc problems start ‘suddenly’, in reality they have probably built up over time; tiny micro-tears can form in discs as we use our spines. If these tears develop in one particular region, a disc bulge can result.
Ultimately, repeatedly using a poor lifting technique can increase your likelihood of a disc problem.
Aging changes are caused by… yep, aging! But having a manual job or playing a lot of sport earlier in life may accelerate those changes.
Sitting in a poor chair for long periods of time (often at a work desk), an imbalance in the hip muscles or tightness in a certain region of the hips can cause piriformis syndrome. These issues have usually been present for a long, long time – you just aren’t aware because the problems never caused you pain before.
Best and worst time of day?
This varies for everyone, but there are a few common patterns. For example, piriformis syndrome rarely causes any pain at night and doesn’t usually wake people up. However, disc problems often do disturb sleep and getting comfortable can be a real challenge.
For aging changes and disc problems, it’s possible that early mornings will be the worst time (for the first 15-60 minutes of the day). With piriformis syndrome, the pain is usually based upon activity rather than a specific time of day. So even though it might feel like your pain is worse in the middle of the day, that might just be because that’s when you’re sitting at work and the chair isn’t helping the problem.
The best time of day for sciatica from aging changes is often mid-afternoon to evening, when the body has had chance to warm up a bit.
Risk factors…?
Because sciatica is highly affected by levels of inflammation in the body, the way we live our lives will be a huge factor in the risk, severity and recovery of this condition.
This has never been truer than with disc problems. Smoking, drinking and eating poorly are all huge risk factors for a disc problem. Equally, poor sleep and being obese will also increase the chances of this problem.
In fact, the risk of suffering from any cause of sciatica is increased by being overweight. This includes piriformis syndrome – more force through the pelvis means the muscles have to work harder and weaknesses get exposed more easily. Click here for a guide to losing weight when you have sciatica.
The likelihood of suffering from age-related sciatica is increased by past spinal surgeries as well as the occupation you once did, as we spoke about before.
Back pain…?
Now, here’s an interesting one.
Some people in my profession say: “It’s simple: back pain = disc problem, no back pain = piriformis problem. Duh.”
Not so fast, genius. For most people, it’s not that simple.
You see, you can have sciatica from a disc problem or aging changes and NOT suffer from back pain at all. It’s well documented in the evidence and I’ve seen it in clinic on countless occasions.
I have some clients who come to me with a “calf strain” – their only complaint is a nagging, burning pain in the calf. After a few tests, it becomes apparent that moving their back aggravates their calf, even though they don’t have back pain. This is a classic example of sciatica from a disc problem with no back pain.
The opposite is also true. I’ve met people with piriformis syndrome before – yet they still suffer from back pain. The back pain they suffer could be from a separate issue entirely, or could even be referred UP into the back from the hips!
Confused yet? I don’t blame you!
But hopefully you can see that just because you don’t have back pain doesn’t necessarily mean your back isn’t the problem, and vice versa.
Summary
So there you have it – the differences between sciatica caused by a back problem and sciatica caused by piriformis syndrome.
I hope I’ve shown here that there’s no exact science to working it out – and a lot of it is an ‘educated guess’ a lot of the time based on the overall picture of your symptoms and how it started in the first place.
Stay tuned for a post soon where I discuss the differences between sciatica and piriformis syndrome treatment!
And now, let me ask: What has your experience with sciatica been? Does the information in this article match up to what you went through? Leave a comment below and let me know!
Are You Looking for RAPID Relief from Sciatica?
My good friend, colleague and fellow international sciatica expert, Dean Volk, has a brand new sciatica relief video course available – and I’m delighted to be an official sponsor!
Check out Dean Volk’s “Kicking Sciatica OUT of the Butt!” Online Pain Relief Course Here!
I can proudly recommend Dean and his course for sciatica sufferers – because I’ve seen his incredible results first-hand. You can check out his course (and get lifetime access to the videos and bonus content) by clicking HERE.
The information on Overcome Sciatica should never be used as a substitute for medical advice from a doctor. Never put into action any tips or techniques from Overcome Sciatica without checking with your doctor first. Please see full terms of use here.