If you’re here reading this, it is likely that you’re suffering from a herniated disc and you’re wondering whether or not surgery is the right option for fixing it. Or maybe you’re just curious. Well, either way, this article will offer some guidance on when surgery may be the best option if you have a herniated disc.
Before we go any further, consider the following:
Surgery should ALWAYS be a last resort for a herniated disc.
Given the costs, time, and inherent risk of these procedures, opting for surgery should not be taken lightly in any circumstances. The process of agreeing to surgery should be carefully considered and discussed at length with your family, your doctor and your surgeon.
Nevertheless, sometimes surgery poses the only option for pain relief and healing to help you get back to life as normal again. In this article, we will start by describing what a herniated disc is, and then reveal the times when surgery might be a sensible option to aid recovery.
What is a Herniated Disc?
The spinal discs are tough outer shells made of collagen fibres filled with a fluid centre. They sit between each of the vertebrae in our spines, meaning we have 24 spinal discs.
When part of an intervertebral disc has weakened significantly, the disc may split (or “herniate”). When the strong outer fibres of the disc split and herniate, the fluid within the disc leaks out at the region where the injury occurred. This is different from a bulging disc, whereby the outer layer remains intact enough to contain the centre (nucleus pulposus).
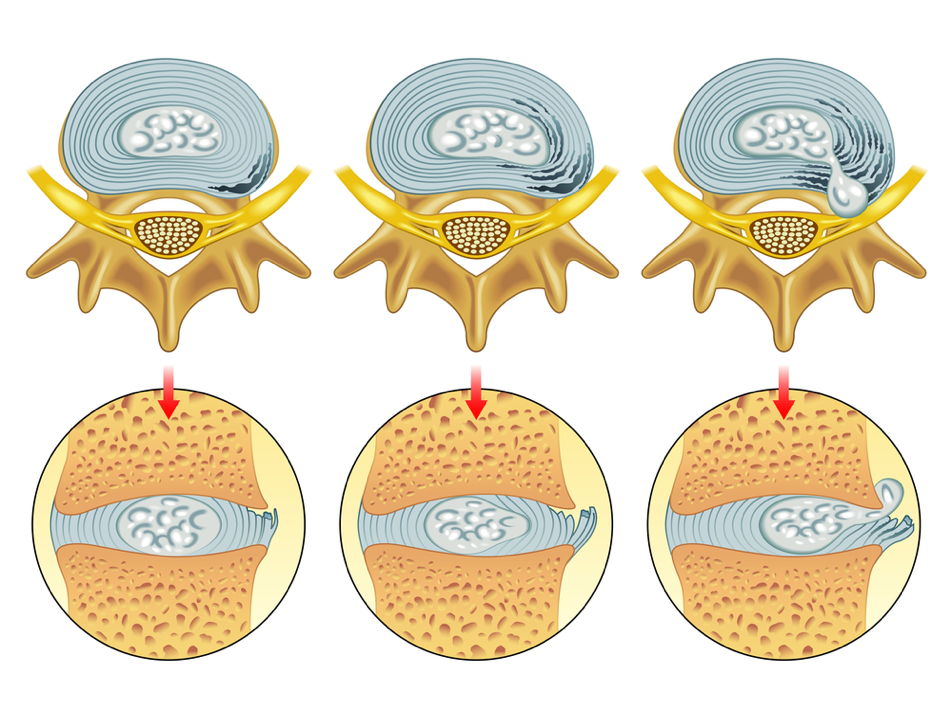
The above shows different degrees of disc damage. The left-hand and middle image show bulging discs, whilst the right-hand image shows a herniated disc.
A herniated disc is more likely than a bulging disc to cause sciatica, as the disc protrudes further, making it more likely to affect the surrounding nerve roots. However, the severity of the injury does not necessarily reflect the severity of the symptoms. The severity of symptoms is usually dictated by the extent to which the surrounding structures are impacted.
When a disc protrudes into the spinal canal, it can end up compressing or irritating your nerve roots. Nerves are incredibly sensitive, and this can cause extreme pain or distortions of the sensations along your nerve channels.
For a detailed guide on the symptoms of a herniated disc, to help you identify if this is what you’re suffering from, please read the following guide.
Can a Herniated Disc be Healed WITHOUT Surgery?
Fortunately, although it will take time and patience, for most people, a herniated disc can heal at home without surgery.
A combination of lifestyle, pain relief medication, rest, and carefully selected exercise can fuel the healing process at home. All the above options should be explored before seeking surgery.
For a full exploration of the lifestyle factors and a detailed list of exercises which can support the healing process of a herniated disc, please see this article.
When Might a Herniated Disc Need Surgery?
Now let’s go over some of the signs that a herniated disc may need surgery:
- Your symptoms haven’t improved after 12 weeks1 : If you have been working on rehabilitative exercises and taking all the right measures to help the problem heal – yet the pain has not improved at all – it might be wise to consider getting a surgical opinion. Please note: The entire process of recovery from a herniated disc can be many months. We would not expect the symptoms to be GONE by the 12-week mark, but we would expect them to be at least improving.
- You are unable to perform daily activities after 12 weeks: this may be the case when the initial injury occurs, but persistent incapacity is an indication that your disc herniation is not healing and/or is causing permanent damage
- Peripheral pain is still present and not moving back towards the spine after 12 weeks: if you’re still experiencing pain in your legs or feet, which is not improving, it is likely the disc is still irritating the nerve roots
- Your doctor identifies the need for surgery following imaging tests (e.g. X-Ray, CT scan, MRI): Imaging is always necessary before going in for surgery and the doctor may pick up on something that is unlikely to resolve without surgical intervention.
- The presence of cauda equina syndrome: This is the most important one and warrants emergency surgery. Cauda equina syndrome is when the herniated disc compresses the nerves at the base of the spine (called the cauda equina), causing symptoms that include (but are not limited to): incontinence, numbness in the “saddle” region, problems initiating bladder or bowel movements, and pain down both legs.
What Surgical Options Exist for Herniated Discs?
Below are the common surgical procedures offered for herniated discs. Your surgeon will be able to discuss the pro’s and con’s of each of these with you.
- Discectomy: surgery to remove part of the herniated disc. The surgeons will focus on removing the protruding parts of the disc to take pressure off the surrounding areas and remove any disc protrusion which may be touching a nerve.
- Disc replacement: although a relatively new advancement, one procedure now possible is the replacement of damaged discs to restore support for spinal movement and stability.
- Laminotomy or laminectomy: there are 10 laminae in the lumbar spine. A lamina is a part of the bone surrounding the spinal cord. Partial segments of a lamina can be removed to relieve pressure on the spinal nerves – this is called a laminotomy. In more extreme cases, an entire lamina may be removed to increase the space around your spinal cord. This is known as a laminectomy (or decompression – which describes the reversal of the nerve compression).
- Spinal fusion: the damaged disc is removed, and the two connecting vertebrae are fused together. For this, bone grafts may be necessary or additional rods or screws to support the joined vertebrae. Although a spinal fusion will render this section of your spine permanently immobilised, this will have limited impact on your overall mobility.
Summary
With a disc herniation, it is important to rest up and explore methods of treatment which can aid the healing process at home.
Remember, ongoing symptoms indicate that surrounding structures have been compromised, which put you at risk of irreversible damage and prolonged pain so be sure to get help if you aren’t improving in a timely fashion. Luckily, surgical options do exist for the unlucky few who need them. If at home treatment unfortunately fails, you should seek professional consultation and explore your surgical options.
Remember that most herniated discs heal without the need for surgery – but the recovery process can take time, effort and patience.
References
- Yoon, W.W. and Koch, J., 2021. Herniated discs: when is surgery necessary?. EFORT Open Reviews, 6(6), p.526.