Sciatica symptoms in the hip is a very common feature of sciatica but it can also be a sign of a completely different issue entirely. Use this handy guide below to find clues as to whether your pain is a sign of sciatica symptoms in the hip or a different problem.
Before we dive in, please be aware that we are part of the Amazon Affiliate programme. This page may contain Amazon affiliate links, so if you choose to purchase a product for your sciatica that we recommend through a link on this page, we will receive a small commission at no extra cost to you. This helps us keep Overcome Sciatica alive! Thank you for your support. Please be assured that we only ever recommend products that we truly believe can help.
How Does Sciatica Cause Symptoms in the Hip?
The term “sciatica” refers to a symptom, rather than a condition. The most common causes of sciatica are disc bulges, aging changes within the spine, and piriformis syndrome.
When we refer to the term sciatica, we usually mean pain in the leg that shoots all the way down from the buttock to the foot.
Sciatica often starts with back pain which then progresses to pain in the hip and leg – but sometimes disc bulges and other problems can cause the pain to start and exist exclusively in the hip, leading to sometimes debilitating sciatica symptoms in the hip.
Why Would Someone Get Sciatica Symptoms in the Hip but Not the Leg?
This is a good question and it generally comes down to the extent that the nerve root in the spine is compressed by a disc bulge or other structure.
The more the nerve root is compressed, the further down the leg the symptoms go.
Equally, the worse the compression, the more likely you are to experience pins and needles or numbness.
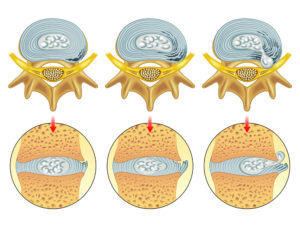
If a disc bulge is just irritating a nerve root and NOT fully compressing it, you might get sciatica symptoms in the hip and back but nothing in the legs.
Another reason for sciatica symptoms in the hip is the muscle tightness that occurs following a back injury. When we hurt our backs, everything “locks up” as the muscles go into overdrive to try and protect the area.
This means that the muscles can effectively go into spasm, which can be extremely painful. If this happens to your buttock muscles, then you can get pain similar to sciatica symptoms in the hips.
What Else Can Cause Sciatica-Like Symptoms in the Hips?
There are many problems that are NOT associated with sciatica that can also cause similar pains in the hip and groin. It is important to know about some of these as they are often treated differently to sciatica.
If you know the key signs and symptoms of the problems that mimic sciatica symptoms in the hip and how you can differentiate them from sciatica, you may find that you can more effectively target treatment towards these other problems.
As always, you should listen to the advice of a qualified health professional rather than attempting to self-diagnose injuries.
Below is a list of many common conditions I see that can mimic sciatica symptoms in the hip. I have included a guide on identifying these problems, who they affect and what you can do about them.
#1 – Hip Osteoarthritis
Commonly referred to as arthritis, this condition simply means aging changes occurring within the hip joint.
Arthritis of the hip is more common than sciatica, with almost half of the population over 60 suffering from some hip-related aches and pains (and almost EVERYONE showing some degree of age-related wear after the age of 40).
How to Identify it:
Hip arthritis usually presents as pain in the groin but can sometimes cause pain on the side of the hip and leg, as is often the way with sciatica. When this condition causes pain on the side of the leg, it can mimic sciatica symptoms in the hip.
The pain will normally be worse with movement and fine at rest, with early mornings and “getting going” from a resting position being the worst times. Along with pain, you may notice restricted movement in the hip, particularly with rotation.
A demonstration of rotation of the hip is shown below. If this exercise gives you pain, you may have hip osteoarthritis:
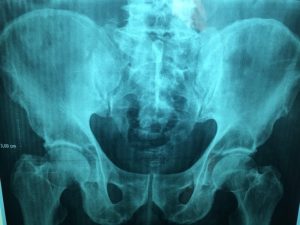
A simple X-ray will likely show the extent of the changes in the hip and can be useful in diagnosis.
Who It Affects:
Hip arthritis usually affects people over the age of 60, but younger individuals can be affected too. Previous accidents or sporting injuries in the hips can make this problem more likely.
How to Help It:
Hip arthritis can be helped somewhat with strengthening and mobility exercises in the hips, depending on how bad the wear to the joint is. If it is a really degenerated joint, you may need surgery like a total hip replacement.
You can try some of the exercises below if you think you may have hip arthritis, but stop if they become painful:
#2 – Gluteal Tendinopathy/Bursitis
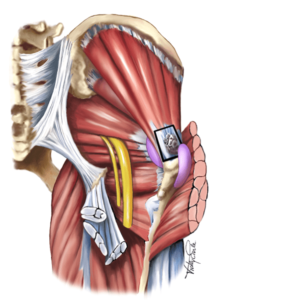
There are many names for this problem (including greater trochanteric pain syndrome, hip bursitis and tendonitis) but they all refer to an issue with either the tendon of the gluteal muscles or the “bursa” that helps to protect it.
A bursa is a fluid sac that helps to protect the tendon. If you have a fall onto one side of your hip and develop extreme pain in this reason, often the cause is a bursitis, or swelling of the bursa.
Over time, the gluteal tendons can begin to degenerate if the muscle they are attached to isn’t strong enough to cope with the demands of your daily life. This causes them to become painful due to tiny micro-tears in the tendon. The pain can be burning in nature, mimicing sciatica symptoms in the hip.
How to Identify It:
This problem will often start gradually and slowly get worse, in a similar way to sciatica symptoms in the hips.
However, there will often be pain when you press on the side of your hip bone. Pain is likely to hurt when walking and may be worse in the mornings.
It may also be particularly bad at night and may make it difficult to lie on your side. (See this guide for improving your sleep with sciatica)
Who it Affects:
This problem affects women much more commonly than men due to the differences in width of the hips between the sexes.
The age group that are usually affected is women in the 40-60 bracket.
How to Help It:
Aside from instances where someone has fallen onto the hip, this condition comes about due to a lack of strength capacity in the gluteal muscles.
Therefore, it can usually be fixed with strengthening exercises.
I used to see clients all the time with this issue and still do occasionally. They had often seen a physio before and been given a hundred exercises to complete – and, like anyone would, they stopped doing any due to sheer overwhelm.
Why give out so many exercises when you only need ONE to fix this problem??
The exercise you need to perform for this issue is shown in the video below:
Just KEEP GOING until you feel the side of your buttock develop a working ache. Doing this once or twice a day is enough to feel some positive results after 1-2 months of work (I’m sorry the results can’t be gained sooner!)
The other thing you should ensure you do is to STOP stretching the gluteal muscles in that hip – stretching these muscles will compress the bursa and the tendon and make your symptoms WORSE.
Stop performing the stretch below, if you are currently doing them and you think you may have this problem:
If your problem started following a fall onto the hip, it should settle on its own after a couple of weeks. But if it hasn’t, your doctor may be able to give you a cortisone injection to calm the painful area down.
I would NOT recommend cortisone injections if your problem started gradually – due to the risk of tendon degeneration and possibility of eventual tearing.
Are You Looking for RAPID Relief from Sciatica?
My good friend, colleague and fellow international sciatica expert, Dean Volk, has a brand new sciatica relief video course available – and I’m delighted to be an official sponsor!
Check out Dean Volk’s “Kicking Sciatica OUT of the Butt!” Online Pain Relief Course Here!
I can proudly recommend Dean and his course for sciatica sufferers – because I’ve seen his incredible results first-hand. You can check out his course (and get lifetime access to the videos and bonus content) by clicking HERE.
#3 – Piriformis Syndrome
Although piriformis syndrome can cause sciatica, it is primarily a problem to do with the hips and buttock.
Piriformis syndrome has NO RELATIONSHIP with disc problems in the back. They exist entirely independently of each other!
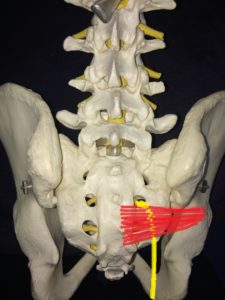
Piriformis syndrome usually comes about slowly as a result of a muscle imbalance between the piriformis muscle, the gluteal muscles and the rotating muscles of the hip joint.
It occurs when the piriformis is over-worked and becomes tight and painful as a result. If this tightness causes the sciatic nerve to become entrapped within the muscle, sciatica symptoms in the hip and leg will result. The image below shows the piriformis in RED and the sciatic nerve in yellow.
How to Identify It:
I have enclosed a FULL guide on identifying, treating and preventing Piriformis Syndrome in all my 90 Day Programmes.
However, here are some quick tips: piriformis syndrome likely starts gradually, is aggravated by sitting for long periods, causes pain predominantly in the buttock (not the side of the hip) and can affect walking, too.
Some people report that they feel like they’re “sitting on a stone” with this condition.
Piriformis syndrome rarely causes problems bending and twisting at the lower back BUT you CAN have back problems and piriformis syndrome at the same time!
Who It Affects:
Piriformis syndrome can affect people of any age but in my experience, it is more common in women aged 40-60.
Piriformis syndrome is most likely to affect people who sit for long periods of time, such as those in office jobs. It can also affect sports people, especially those who do long distance running and walking.
How to Help It:
You can relieve piriformis syndrome by stretching the affected side as long as this is NON-painful.
Try some of the stretches below for great effect:
If stretching the painful side causes your symptoms to worsen, try stretching the OPPOSITE side instead. Although this sounds strange, it can help to re-balance your hips and relieve pressure on the piriformis.
My friend and fellow International Sciatica Consultant, Dean Volk, also recommends performing strengthening exercises on the NON-PAINFUL side for piriformis syndrome.
This is worth trying as recent research shows how there is some carry-over in strength gains from the right leg to the left leg and vice versa, when only one leg is strengthened. The body can be truly amazing!
Try the strengthening exercise below on the non-painful leg. Keep repeating until you feel a “working ache” in your hip:
#4 – Sacro-iliac Dysfunction & Mechanical Back Pain
These two terms are fancy ways of talking about plain old back pain.
When I talk about these two issues, what I’m really meaning is back pain with NO evidence of damage to the back, discs, muscles or ligaments.
This type of back pain may account for over 70% of all the back pain in the world! This is absolutely crazy considering we, as healthcare professionals, still really don’t fully understand it.
There are so many factors that can lead to mechanical back pain, including stress, poor lifestyle choices, muscle imbalances, depression and even too much rest.
However, mechanical back pain is rarely serious and usually resolves within 2 weeks.
Mechanical back pain can lead to sciatica-like symptoms in the hips due to a phenomenon called “referred pain”. This is another concept that we don’t fully understand.
Referred pain occurs when one painful region “fires up” the nerves in another region of the body, causing the pain to spread.
This means that a mechanical (movement) problem in the back can lead to pain that spreads into the hips, even though the hips are moving and working just fine with NO evidence of damage.
Sacro-iliac joint dysfunction (SIJD) is a controversial topic that may or may not be exactly the same as mechanical back pain. We tend to treat it the same way, anyway, which is why I put it in this section.
With SIJD, you will likely feel pain right at the junction between your back and your upper buttock, sometimes over the sacrum (lowest spine bone). The pain may spread or radiate into your buttock.
How to Identify It:
Mechanical back pain may start slowly and gradually worsen over the course of a few days, or it might start following a twist or minor trauma.
This type of back pain never comes with pins and needles or numbness, nor is the pain likely to spread past the lower border of your buttock into the leg. If these symptoms are occurring, true sciatica is the more likely cause of your pain.
Mechanical back pain responds to movement. This means that some movements will be more painful than others. Your pain is most likely to be best when you are completely at rest, for example at night (although some people do get night pain with mechanical back pain).
SIJD may make walking uncomfortable and you may get more pain when standing on one leg, due to the pressure going through the sacro-iliac joint.
Who It Affects:
Mechanical back pain and SIJD can affect anyone but these conditions are more common as we age.
The sexes are equally affected and back pain can affect people in any occupation, although jobs where people sit all day OR carry out manual work all day tend to have the highest occurrences.
The active population who regularly exercise and eat well are least likely to be affected.
How to Help It:
As I mentioned before, most mechanical back pain just resolves on its own within a few weeks. However, if yours isn’t improving, you need to do something about it.
Stretching the legs is a good start. You can see a full stretching programme for back pain by following this link.
Finally, making small changes to your lifestyle can have a huge effect on back pain. If you sit for long periods of time at work, setting an alarm for every hour to get up, stretch and move around for 30 seconds can make a world of difference and is a great habit.
Getting enough sleep and taking up an activity that helps to relieve stress will also contribute to a healthier back.
Walking is GREAT for back pain (as long as it isn’t aggravating your symptoms). If you find walking difficult, try walking in a pool or swimming instead.
Summary
Although there are many other conditions that may cause sciatica symptoms in the hips, these are by far the most common but treatable problems that I see regularly.
If you are suffering from sciatica symptoms in the hips but aren’t 100% sure what could be causing it, it is always best to get checked out by a qualified healthcare professional.
Are You Looking for RAPID Relief from Sciatica?
My good friend, colleague and fellow international sciatica expert, Dean Volk, has a brand new sciatica relief video course available – and I’m delighted to be an official sponsor!
Check out Dean Volk’s “Kicking Sciatica OUT of the Butt!” Online Pain Relief Course Here!
I can proudly recommend Dean and his course for sciatica sufferers – because I’ve seen his incredible results first-hand. You can check out his course (and get lifetime access to the videos and bonus content) by clicking HERE.
The information on Overcome Sciatica should never be used as a substitute for medical advice from a doctor. Never put into action any tips or techniques from Overcome Sciatica without checking with your doctor first. Please see full terms of use here.
As always, thanks for reading.