As more and more evidence comes out it is clear that, over the long term, medications, injections and surgery are not controlling the worldwide back pain and sciatica epidemic. Let’s have a look at some alternative options…
Aims of this post:
- To compare the reliable evidence about massage, manipulation and acupuncture
- To talk about how you can find what’s best for YOU
- To suggest alternatives to these popular treatments
- To talk about my own experience with these treatments
Before we dive in, please be aware that we are part of the Amazon Affiliate programme. This page may contain Amazon affiliate links, so if you choose to purchase a product for your sciatica that we recommend through a link on this page, we will receive a small commission at no extra cost to you. This helps us keep Overcome Sciatica alive! Thank you for your support. Please be assured that we only ever recommend products that we truly believe can help.
Failed Treatments
The longer I work, the more I hear stories of failed surgeries, people addicted to opiates and injections that did nothing except cause significant trauma and cost to the patient and/or healthcare system.
I’m certainly not alone in this regard. Many people are realising that the traditional medical route is not very effective on the whole for back pain and sciatica. Sure, some people get great results with surgery and there are some situations where surgery is needed, such as in cauda equina syndrome. But for 2 out of 3 people who opt for surgery for back pain and sciatica, their pain stays the same or gets worse.
For this reason, it is important for people with sciatica to consider alternative options.
To read more about surgery, who it can help and who should avoid it, click HERE!
Alternative Options
Three of these alternatives stem from the therapist’s toolkit. Spinal manipulation, acupuncture and massage are commonly used by physiotherapists, chiropractors and osteopaths, but what’s the evidence for their effect?
Do they help to alleviate back pain and sciatica?
Can they make the problem worse?
Let’s have a look at each one, with an honest review of the evidence, and decide what might be a good way forward for YOU.
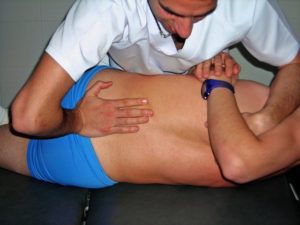
Spinal Manipulation
How it works
Spinal manipulation is the act of taking a joint in the spine to end range, and sometimes past end range, with a quick thrust. It is often accompanied by the audible click or pop that comes to mind whenever someone mentions the word “chiropractor”.
Those on my mailing list will have recently read on Three-Tip Thursday that this pop is not actually bones crunching together or realigning; rather, it is gas escaping from the joint capsule due to the rapid pressure change.
These clicks are also harmless and WON’T lead to arthritis.
Weak Evidence
The research base for spinal manipulation is also generally weak. Unfortunately, there are inevitably vested interests in the results of the studies, too, when you read that a practitioner who invests heavily in this type of treatment is the experimenter in the study.
There’s a lot of variability among the practice styles and standards of treatment, as well as levels of experience. It can be difficult to blind the patients to the treatment they are receiving (you are either cracked or you aren’t!), and the people who seek out spinal manipulation may be more likely to believe they are truly “healed” by the hands of a therapist.
However, there are some summary points we can take from the available evidence.
There is some evidence the approach can help people with chronic back pain — but not any more than over-the-counter painkillers or exercise. A 2011 review (Rubinstein et al.) on chronic low back pain found that spinal manipulation had small, short-term effects on reducing pain and improving functional status.
The review on acute (less than 6 week’s duration) pain found that spinal manipulation worked no better than placebo (Rubinstein et al., 2012). This suggests that people with a short episode of back pain should probably not bother seeing a therapist.
Why? Possibly because 90% of back pain resolves independently within 6 weeks. Chances are, if you’re reading this post you have suffered for far longer than 6 weeks so won’t necessarily be in this category anyway.
Are You Looking for RAPID Relief from Sciatica?
My good friend, colleague and fellow international sciatica expert, Dean Volk, has a brand new sciatica relief video course available – and I’m delighted to be an official sponsor!
Check out Dean Volk’s “Kicking Sciatica OUT of the Butt!” Online Pain Relief Course Here!
I can proudly recommend Dean and his course for sciatica sufferers – because I’ve seen his incredible results first-hand. You can check out his course (and get lifetime access to the videos and bonus content) by clicking HERE.
My Own Experience
Personally, I find manipulation useful for lower back pain, but I am VERY cautious when using it with people suffering from sciatica.
The idea of taking a joint to end range in a quick thrust in someone who has an inflamed, angry nerve root does not sit well with me.
I would rarely, if ever, perform manipulation on someone with sciatic pain travelling past their knee. This is just something to bear in mind if you are seeking this type of treatment.
I have also heard of many occasions where manipulation has REALLY aggravated someone’s sciatica symptoms for a short period of time.
You need to take precautions when seeking out a therapist to perform these techniques on you, making sure they are qualified to perform them and experienced with back pain and sciatica.
Be Wary
The other thing to be wary of is long, drawn out plans of care from manual therapists. People who respond well to these techniques tend to do so quite quickly, so if you’re being asked to come in twice a week for twelve weeks, it might be best to reconsider!
Some chiropractors are able to order x-rays; be wary of these when it comes to back pain, as they are no good at diagnosing the cause of back pain.
Doctors will no longer routinely order spinal x-rays for this reason.
Although the cracks and pops during spinal manipulation are dramatic, it is actually incredibly safe. The risk of serious complications from the manipulation of the lower back is about 1 in 10 million.
However, the rate of serious adverse events is higher when the neck is manipulated due to the risk of stroke.
So, in summary, spinal manipulation is about as effective as exercise and over-the-counter drugs for the treatment of back pain, while the jury is still out with regards to its efficacy for sciatica.
Massage
How it works
In general, massage works through manipulating the muscle and soft tissue of the back. There are many different styles of massage and they vary in how long they last, pressure used and frequency, which makes the evidence for massage pretty difficult to interpret.
Researchers who study back pain say the approach makes sense from a pain relief perspective – by “releasing” tight and wound up structures, the pain around an area can decrease.
Massage may also affect us on a neurological level, adapting the way that pain messages are interpreted by the brain.
To read about how the brain affects sciatica, click HERE!
Bervoets et al., (2015) states that in subacute (lasting between seven and 12 weeks) and chronic low back pain, massage can improve symptoms and function in the short term — but there’s no evidence that it leads to any long-term change. In layman’s terms, you’ll get a bit of immediate relief, but nothing lasting.
More weak evidence!
The Cochrane review (Furlan et al., 2015) on massage treatment for low back pain looked at 25 trials on massage, finding short-term improvements in pain and function for both subacute and chronic low back pain. However, again, the trials they included in their review were of mixed quality from a research methods perspective.
The good news
The difference between the treatments of massage and manipulation is the level of risk involved. There have been far fewer instances of serious adverse events from massage compared with spinal manipulation.
One good thing about massage is that you don’t necessarily need to run to the phone book and look for your nearest massage therapist; you can perform some of the common techniques at home, all by yourself. All you’ll need is a hard ball or foam roller.
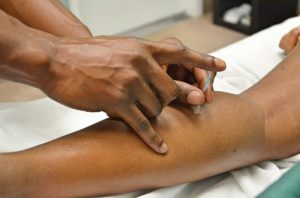
Acupuncture
How it works
As a core part of traditional Chinese medicine, acupuncture has been used for centuries by the Far East to treat a variety of musculoskeletal ailments.
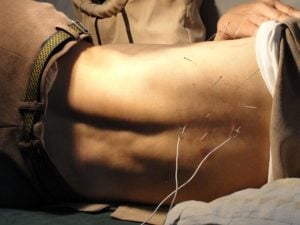
Essentially, acupuncture is the act of placing needles into areas of the body. The philosophy behind why we do this depends on who you listen to; if you are following the traditional Eastern approach, the needles are supposed to stimulate “meridians” in the body. This is supposed to balance the “Yin and Yang” forces of the body, which has the potential to modulate health and illness.
However, the Western approach is far less grounded in spirituality – so called “dry needling” is performed which involves sticking the needles into tight areas of muscle tissue, to bring healthy blood to the area and encourage tight spots to relax.
How did it perform in trials?
A 2005 Cochrane review (Furlan et al., 2005) into acupuncture and low back pain found there was “insufficient evidence” to make any recommendations about acupuncture for acute low back pain — so the jury is still out if you’ve suffered for <6 weeks.
For chronic back pain, acupuncture seemed to offer more pain relief and functional improvements when compared with no treatment or sham acupuncture (when practitioners use needles that don’t actually penetrate the skin). However, acupuncture was no more effective than other treatments.
Still, the evidence for acupuncture’s effects on chronic pain is somewhat conflicting. The Cochrane review also noted it was unclear whether acupuncture’s benefit lies in the needling, or in the placebo effect.
Placebo effect?
Cherkin et al., (2009) found that acupuncture seemed to reduce chronic low back pain — but they also observed the fact that it didn’t make a difference as to where the needles were placed! This study places the traditional acupuncture methods under scrutiny undoubtedly, but the changes seen were deemed to be clinically relevant, so acupuncture may be worth a go if you have suffered for >12 weeks.
This is what makes acupuncture controversial. Science suggests it might work, sometimes, in some people… But we can’t yet predict who it will or won’t work for.
Undoubtedly, acupuncture elicits a certain theatrical effect over a patient – and we know that the more dramatic the medical intervention, the stronger the placebo effect.
However, with that being said, I have had patients with back pain and sciatica that greatly benefitted from a short course of acupuncture. Even though the latest NICE guidelines do not recommend the use of acupuncture for the treatment of low back pain or sciatica, I would still certainly consider using it (but probably only if my primary interventions failed).
Summary
To summarise, the research suggests that all of the above treatments have potential to help some people, some of the time. For this reason, they are certainly worth considering. They are generally low-cost, low-risk and can be seen as “natural alternatives” to medication.
However, it’s important to remain realistic. None of these treatments are being sold as a “fix” for back pain or sciatica, and the positive effects seen from them are at best moderate.
It’s worth talking about the other natural intervention that we didn’t think about here – exercise – which performs as well as, if not better than, the above interventions in every trial I know of.
As always, thanks for reading.
The information on Overcome Sciatica should never be used as a substitute for medical advice from a doctor. Never put into action any tips or techniques from Overcome Sciatica without checking with your doctor first. Please see full terms of use here.
References
Bervoets DC, Luijsterburg PAJ, Alessie JJN, Buijs MJ, Verhagen AP (2015) Massage therapy has short-term benefits for people with common musculoskeletal disorders compared to no treatment: a systematic review.Journal of Physiotherapy 61: 106–116
Cherkin, D.C., Sherman, K.J., Avins, A.L., Erro, J.H., Ichikawa, L., Barlow, W.E., Delaney, K., Hawkes, R., Hamilton, L., Pressman, A., Khalsa, P.S., Deyo, R.A. (2009). A randomized trial comparing acupuncture, simulated acupuncture, and usual care for chronic low back pain. Arch Intern Med. 169(9). 858-866.
Furlan, A.D., van Tulder, M.W., Cherkin, D.C., Tsukayama, H., Lao, L., Koes, B.W., Berman, B.M. (2005). Acupuncture and dry needling for low back pain. Cochrane Database Syst Rev. 25 (1).
Furlan, A.D., Giraldo, M., Baskwill, A., Irvin, E., Imamura, M. (2015). Massage for low-back pain. Cochrane Database of Systematic Reviews. Issue 9.
Rubinstein, S.M., van Middelkoop, M., Assendelft, W.J.J., de Boer, M.R., van Tulder, M.W. (2011). Spinal manipulative therapy for chronic low-back pain. Cochrane Database of Systematic Reviews. 2.
Rubinstein, S.M., Terwee, C.B., Assendelft, W.J.J., de Boer, M.R., van Tulder, M.W. (2012). Spinal manipulative therapy for acute low-back pain. Cochrane Database of Systematic Reviews, Issue 9